Telehealth
Everything you need to know about our telemedicine services.
We have been actively involved in the Telemedicine since 2014. Our experience has included telephonic, video visits, remote patient monitoring and deployable equipment to an individual’s homes.
What Is Telehealth?
Telehealth is a method of delivering clinical health services to patients at a distance using interactive audio and video telecommunication.
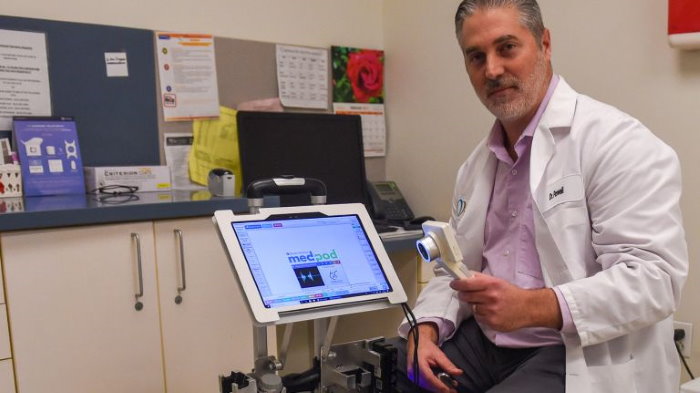
It is often used as an umbrella concept to encompass more narrowly defined care such as telemedicine, store and forward and remote patient monitoring. In general though, telehealth helps people get access to the care they need by overcoming the barriers of distance, time, quarantining, stigma, and/or the patient’s own lack of mobility.
The range of telehealth use is broad and growing constantly. Examples of video enabled telehealth include:
- At home, using a secure video connection to enable a patient to use their smartphone or tablet to talk to their psychiatrist from their own sofa, follow up with the cardiologist, or obtain treatment for sunburn or poison ivy.
- At school, enabling a doctor to triage a student who fell ill to determine whether to send him to the hospital.
- In an Emergency Department at the hospital, enabling the patient to be examined by a specialist in another city.
- In a locked down assisted living facility during the COVID emergency, enabling the nurse practitioner to continue to “see” patients for medication checks, follow ups, assessments and therapy sessions.
Remote patient monitoring (RPM) is a rapidly growing aspect of telehealth. RPM gives the clinical team regular — even continuous — readings from the patient, using devices that remain in the patient’s home. An RPM kit contains a tablet and the devices that are relevant to the patient’s condition, which could include a blood pressure monitor, a scale, a thermometer, a pulse oximeter or a glucose reader. The tablet sends patient readings to the provider’s clinical dashboard, delivers provider-generated messages back to the patient, and enables video visits. Typical kits are designed to monitor diabetes, hypertension, COPD, obesity, congestive heart failure and the like. Today, we are gearing up to issue COVID kits, which will include a digital stethoscope and a digital thermometer. This will enable us to monitor respiratory symptoms of infected individuals to determine whether they need to be hospitalized and provide treatment as they recover.
What Services Does Telehealth Provide?

Telehealth can be used to provide just about any type of service that doesn’t require the doctor to smell or touch the patient.
Our telehealth doctors know that if they can put eyes and ears on someone, they can address 60-70% of what patients present with.
We’ve used telehealth to diagnose pneumonia, treat an entire group home for scabies, treat heartburn, diagnose shingles and assess individuals after a fall.
Our psychiatrists, psychologists and social workers all conduct therapy sessions using video.
What Is the Difference Between Telehealth and Telemedicine?
Telemedicine is a subset of telehealth. Its definition requires two-way, synchronous electronic audio-visual communication to deliver clinical health care services to a distant patient that is of an amount and nature that would be sufficient to meet the key components and or requirements of the same service when rendered face to face. This distinction matters primarily for the purpose of insurance reimbursement. Our team’s focus is on using the best and most effective approach to address the need, based on resources and the technology at our disposal.
Why Is Telehealth Especially Important During the COVID-19 Crisis?
It’s helping keep patients, health care workers and the well public safer.

Telehealth enables doctors to see and treat individuals who are:
- at home with virus symptoms, to monitor them and keep them out of the hospital
- quarantining, to keep them isolated
- ill or needing care for non-COVID issues, to keep them from being exposed to the virus
- concerned about whether their injury, toothache, migraine headache or other ailment requires a trip to the Emergency Room.
Telehealth supports social distancing by letting healthy people, or people with non-virus conditions, receive primary and urgent care without leaving home. This is critical with so many hospital beds and emergency room bays needed for virus victims.
Is Telehealth Covered by Insurance?
Medicaid and Medicare instituted changes in March and April to regulations to encourage telehealth use for this emergency period. Commercial insurers are following suit. In addition, many insurance carriers are offering access to telehealth through their own websites, for a fee.
Ask your doctor’s office whether they are providing telehealth as an alternative to an in-clinic visit, and whether it will be covered. Call your insurer to ask about telehealth coverage or go online to see your covered benefits. They may have updated their websites to reflect the answer to your questions.
Can Patients File for a Reimbursement if Their Telehealth Visit Isn’t Covered
Many insurers have sent us letters letting us know that they will be covering telemedicine services until this crisis is over. We recommend if a patient is not sure about coverage they will have to reach out to their individual carrier for a clear answer.
What Happens During a Telehealth Appointment?
A medical telehealth appointment is a lot like doing FaceTime or WhatsApp with your doctor or nurse.

You log into an app or a website, and when the doctor comes on the screen, both parties can see one another. Your doctor will see and speak with you, conduct the visit, and conclude it.
If you need a prescription, your doctor will order it. A therapy session will be conducted the same way — like a Zoom meeting.
How Can Patients Prepare for Their Appointment?
A strong wifi connection is essential. Prior to your appointment find a quiet, private, well lit spot in your location that will enable you to do a video visit. You don’t want others walking through the room or playing loud music while you are conducting a visit. Have with you any notes, questions, lab results, or other items that you need to talk about with the doctor. If you are seeking help for something like a sore toe or a rash on your back, be prepared to show the area to the doctor. Be sure you understand what the doctor or clinic will do if your visit is cut short, which may be to call you, so be sure they have your phone number.
What Happens if a Diagnosis Can’t Be Made Via Telehealth?
Then the medical professional conducting the visit will determine the correct course of action, which may be to send you to the hospital or have you come to the clinic the next day. Telehealth is an excellent way to determine whether a trip to the Emergency Department is really necessary, especially now during the COVID crisis. In fact, where possible the telehealth doctor can call ahead to communicate their observations to the ED or ambulance team before the patient arrives.
Can Medication Be Prescribed Via Telehealth?

Generally, yes. This is true whether the prescribing provider has a pre-existing relationship with the patient or not. Just this week, the DEA relaxed provisions regarding prescribing controlled substances via telehealth and telephone during the crisis.
Does Telehealth Include Phone Consultations?
Until the advent of the COVID crisis, telehealth reimbursement from Medicare and Medicaid did not clearly and consistently include providing care by phone. This too has been relaxed during the crisis.
What Are Some of the Benefits and Limitations of Telehealth?
The benefits are that care can be delivered by a provider located anywhere to a patient located anywhere, at any time of day or night. Care and intervention does not have to be in real time – for example, a patient can send a photo of a rash or a blood pressure and heart rate reading for interpretation by the provider. The provider can send a set of questions, instructions or educational materials that can be reviewed by the patient ahead of a scheduled appointment.
The biggest limitations are:
- Lack of wifi access and bandwidth that limits connectivity in both rural and urban settings
- Lack of ability to put hands on the patient
- Fear of the new
Conclusion
Telehealth profoundly changes the way health care is understood, practiced and consumed. We are still primarily retrofitting traditional medicine with technology. But in reality, health care is becoming part of the internet of things. The tragedy of COVID-19 has galvanized the mainstream use of telehealth, and there will be no turning back.